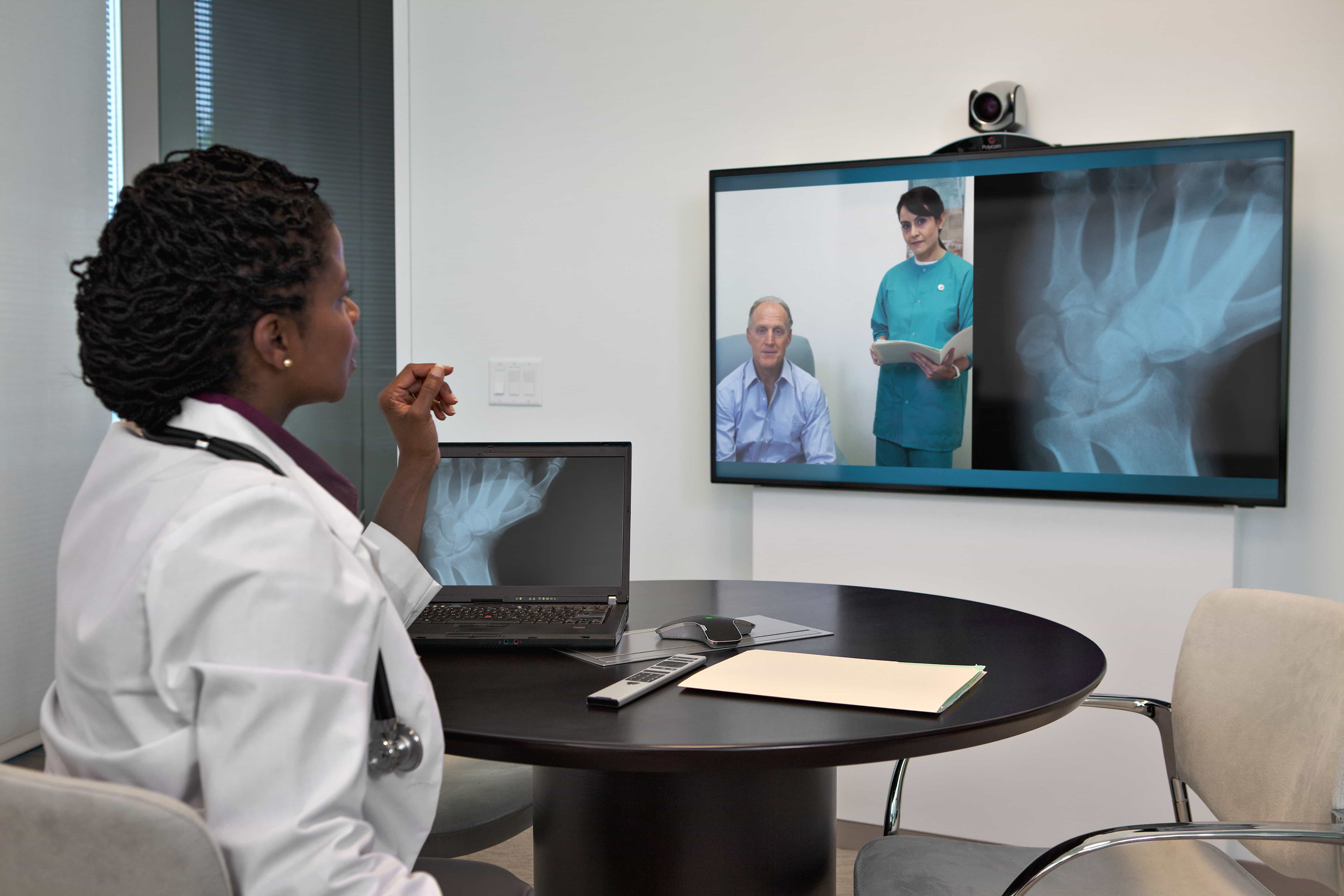
Telemedicine and telehealth change the reality of health in Brazil
Whenever she needed to do an eye examination, seamstress Ana do Nascimento used to wake up before sunrise, take a bus that took two hours to get to downtown Goiânia and spend the entire morning in a public hospital, waiting for her turn to be seen by an ophthalmologist who could verify her degree of myopia.
She arrived home in the afternoon, tired and not always satisfied. Today, the “examination day” is no more than 30 minutes. Ana only needs to go to the health center of the municipality of Morrinhos, where she lives, to be seen.
Introducing telehealth
The new reality is due to the benefits of telehealth, which offers healthcare services and attention remotely, through Information and Communication Technologies (ICT) and to the work of professionals who, regardless of where they are, exchange information regarding the patient, through video or web conferences, aiming to analyze the case and reach the final diagnosis.
In Brazil, the change in the routine of many Brazilians, whether they are patients or doctors, is justified due to two public initiatives in the health area: the Brazilian National Telehealth Network Program (“Telessaúde Brasil Redes”) and the Telemedicine University Network (Rute).
Launched in 2006, the Brazilian National Telehealth Network Program is a program by the Ministry of Health (MS), which aims to improve quality of service and primary care in the Unified Health System (SUS), through ICT tools, which enable the promotion of tele assistance and tele-education.
The action is present throughout Brazil and allows the qualification of Family Health professionals and the exchange of information via internet between SUS doctors and experts, through the offer of tele-diagnosis and tele-consultancies on clinical cases, work process, health education, planning and monitoring of actions in primary health care.
Rute also emerged in 2006, as an initiative by the Ministry of Science, Technology and Innovation (MCTI), to deploy communication infrastructures at public universities and their university hospitals (UHs), health institutions and certified education and research hospitals in the country, benefitting the creation of Telemedicine and Telehealth cores.
NREN co-ordination
Coordinated by RNP, the network strengthens and integrates the Brazilian National Telehealth Network Program by enabling exchanges between health professionals and national research groups, through the sharing of information, lectures, lifelong learning actions, formative second opinion and tele-consultancies.
It also has 55 Special Interest Groups (SIGs) in various health specialties, which gather to discuss clinical cases and exchange experiences and knowledges. Currently, Rute is comprised by 118 units in full operation in the five regions of Brazil, and covers over 150 institutions.
Equipped with cutting edge equipment for real-time communication, the Telehealth and Telemedicine cores are connected to the high-performance infrastructure operated by RNP, the Ipê network. Currently, they serve approximately seven thousand teams from the Family Health Program, in over one thousand Brazilian municipalities.
The benefits of telehealth and telemedicine
In Rio Grande do Sul, the videoconference resources were used to help the victims of the fire at the Kiss nightclub, in the city of Santa Maria, in January 2013. Virtual meetings were held between the Ministry of Health, the National SUS Force, the Brazilian hospitals, especially those from the South that assisted the wounded, and reference centers in training of lung burns, such as those in Iraq, Miami, Toronto and San Diego, to define strategies for the treatment of the patients.
“The Santa Maria health teams had our support in the psychological treatment of the victims of the fire and the relatives, since incidents such as this hit close to the emotional side”, Erno Harzheim, coordinator of the telehealth core of the Federal University of Rio Grande do Sul (UFRGS), remembers.
In Rio de Janeiro, in the Telemedicine core of the National Institute of Traumatology and Orthopedics (INTO), there is the partnership with the Brazilian Olympic Committee (COB) for the discussion, via videoconferences, of clinical cases of more complex lesions of athletes during the Olympics. In 2012, in London, the medical teams of Brazilian delegations received help from experts from the INTO orthopedic surgery centers.
“We gave support during the Olympic games”, coordinator Marisa Peter Silver says. “We will also participate in the organization and performance of large events in Brazil”, she reveals. In the 2016 Olympics, the focus of the work will also be the second medical opinion.
In Goiás, almost 500 ethnographies are examined monthly, detecting the main causes of blindness at an early stage. An important work in the ophthalmology area is performed through tele-diagnosis.
“The patients go to the health center, do the necessary sight exams and wait for the result. The captured images are sent to a central, so the specialized ophthalmologist doctor makes the diagnosis. After the report is done, he sends it to the health professional caring for the patients at the center. If it is a serious case, the recommendation shall be to visit an ophthalmologist. Otherwise, it shall only contain the indication for treatment”, explains Alexandre Taleb, coordinator of the telehealth and telemedicine core of the University of Goiás.
In Amazonas, the deployment of the National Telehealth Program and Rute’s telehealth and telemedicine cores narrowed the geographic access barriers and the lack of professionals for assisting with health in the state, overall in the countryside, in areas of riverside population and indigenous community. The telecommunication is done through radiofrequency antennas spread through the basic health units distributed across the Amazonian territory, which integrate local health professionals to the central core of the University of the State of Amazonas (UEA). The indigenous health work is highlighted among the telehealth actions in the Amazonian region.
“Our indigenous population may be the largest in Brazil. In addition to getting closer, we had to know the reality in which they live”, says Cleinaldo Costa, coordinator of the Amazonia telemedicine pole and current dean of UEA.
In Amazonas, there are two telehealth poles in Brazilian indigenous areas, one located at the district of Iauaretê, in the municipality of São Gabriel da Cachoeira, in the extreme northwest of the State, and another in Umirituba, in the municipality of Barreirinha, 372 km away from Manaus, or a 6h trip – 4h30 using a “voadeira”, small craft used by the riverside population, to reach Parintins, and 1h30 by plane from Parintins to Manaus.
Currently, approximately five thousand indigenous people are attended by health professionals in Umirituba. At the indigenous areas, most tele-care is associated with skin diseases and ailments caused by alcoholism, such as liver cirrhosis, diabetes and high blood pressure.
“In addition to the indigenous communities, with the telehealth infrastructure, in five years, we had the opportunity to care for over 75 thousand people. It is a considerable number, because people would have to resort to SUS in Manaus,with a very high cost of travel and often by air”, Cleinaldo explains.
In Minas Gerais, telehealth care is provided to 710 municipalities (83% of the state), corresponding to almost one thousand service points, benefitting almost 1,900 Family Health teams. Approximately 60 thousand tele-consultancies were performed, and, in the area of tele-cardiology, the State beat the record of over 2 million electrocardiograms analyzed from a distance.
The Telehealth Center of the Clinical Hospital of the Federal University of Minas Gerais (UFMG) coordinates the Tele-assistance Network of Minas Gerais (RTMG), a partnership by six public universities from Minas Gerais that became an example of sustainable, large-sized telehealth service. Currently, approximately two thousand electrocardiograms are analyzed daily.
In addition, the patient does not need to have any transportation, food and lodging expenses, if necessary. Beatriz Alckmin, coordinator of the telehealth core of the UFMG Clinical Hospital, stresses the benefits of the technology.
“On average, 80% of the tele-health consultations avoid the referral of patients, which generated savings for the public health system of approximately R$ 80 million in eight years of operation, proving the economic viability of the practice”.
Another highlight of the tele-cardiology area is the participation of the service in the Acute Myocardial Infarction (AMI) Care Network, in Belo Horizonte. The results reached allowed to develop the Minas Telecardio 2 project, which is deploying the AMI Care Network to the North of the State, with the installation of electrocardiograms in ambulances of the Mobile Urgent Care Service (SAMU) and in regional hospitals to improve the caring for patients with suspected AMI in remote, isolated areas.
In Pernambuco, the telehealth core of the Federal University of Pernambuco (UFPE) makes available tele-education, tele-assistance and tele-management services. According to coordinator Magdala Novaes, there is a great performance also in the area of research and development.
“It is one of the strongest areas, because we develop technologies and we evaluate their impact in improving the quality of health care for the population, while also contributing to training of specialized human resources in digital health”, she says. Another strong feature is the work performed in the area of blood policy.
The core developed and deployed the Rhemo Network, of virtual videoconference collaboration for the hemotherapy and hematology services in the country, in partnership with the General Blood and Hemoderivatives Coordination of the Ministry of Health. Thirty one videoconference rooms were deployed at every coordinating blood centers of Brazil.
“This network’s goal is to contribute to increase the efficacy of management processes, exchange of experiences, support to research and formation of knowledge networks among the services of the Brazilian hemo-networks, and their integration with the other telehealth networks of the country, such as Rute and the Brazilian National Telehealth Network Program.
“Through videoconferences, clinical and managerial meetings, courses and seminars take place from north to south, enabling the improvement of diagnostic techniques and permanent professional development in every Coordinating Blood Center of the country”, Magdala explains.
According to the National coordinator of the Telehealth Brazil Networks, Tâmara Guedes, the program is gaining visibility. “It is becoming a focus of interest by the management from the evidences presented, becoming an important regulatory tool. The Telehealth acts in the reduction of referrals to specialties, reducing waiting lines for care and costs for management”.
These results were seen in focal studies performed by the cores of the State of Minas Gerais and by the State of Rio Grande do Sul, which show that tele-consultancy is able to avoid, in approximately 70% of the cases, the need for removal of patients, because these are resolved in the same Family Health units.
A satisfaction research with the teams that use the service attested that 67% of the professionals believe telehealth to contribute largely to disrupt the sense of isolation and for their decision to remain in remote locations.
“The growth of Telehealth since its inception in 2006 is noticeable. From the amount of points deployed, the growth in the use of services to its complex cores network.
“The results achieved with the implementation of the program and Rute demonstrate a significant progress in the qualification of health professionals, especially those working in the municipalities of difficult access,” Tâmara concludes.
For more information please contact our contributor(s):

